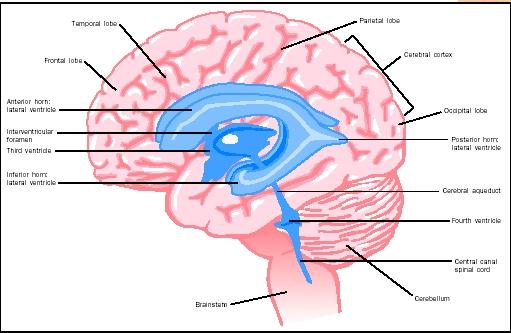
Cortical inflammatory lesions (Grey matter lesions in the cortex (outerlayer) of the brain) have been correlated with disability and cortical atrophy in multiple sclerosis. The extent to which cortical lesion load is associated with longer-term physical and cognitive disability in different multiple sclerosis
phenotypes has not yet been investigated.
Thus, a 5-year prospective longitudinal study was carried on in a large group of patients with multiple sclerosis. Three hundred and twelve consecutive patients with multiple sclerosis (157 relapsing remitting, 35 paediatric, 45 benign, 44 primary progressive and 31 secondary progressive) were enrolled in a 5-year prospective clinical and neuroimaging study. Several magnetic resonance parameters (including cortical lesion number and volume, contrast-enhancing cortical lesions and grey matter atrophy) were analysed to find associations with clinical and cognitive outcomes.
Patients with high cortical lesion load (a lot of Grey matter lesions) had higher Expanded Disability Status Scale increase (median = 1.5; range = 0-3. More movement disability) during the study than both patients with low cortical lesion load (median = 1.0; range = 1-3, P < 0.001) and without cortical lesions (median = 0.5; range = -1 to 2, P < 0.001). Compared with clinically stable patients, 101 (32.4%) patients showing clinical progression at 5 years had the highest rate of cortical lesion accumulation (P < 0.001. The more active is your MS the more disability that is accumulated). Stepwise regression analysis revealed significant and independent contributions from age (β = 0.55), cortical lesion volume (β = 0.58), T2 white matter lesion volume (β = 0.34) and grey matter fraction (β = 0.42) as predictors (final model with r2= 0.657, P < 0.001) of Expanded Disability Status Scale change (Age, Size of White and Grey Matter lesions are predictors of mobility). Disease duration (β = 0.52, P < 0.001), cortical lesion volume (β = 0.67, P < 0.001), grey matter fraction (β = 0.56, P < 0.001) and T2 white matter lesion volume (β = 0.31, P = 0.040) at baseline were found to be independent predictors of cognitive status at the end of the study (The longer you have had disease and grey and white matter lesion load are predictors of disability years later)
While confirming the relevance of cortical pathology in all multiple sclerosis phenotypes, but benign, our study suggests that grey matter and white matter changes in multiple sclerosis occur, at least, partly independently, and that grey matter, more than white matter, damage is associated with physical and cognitive disability progression. Thus, the combination of grey and white matter parameters gives a more comprehensive view of multiple sclerosis pathology and allows a better understanding of the progressive phase of the disease, which, however, seems more related to cortical damage than to subcortical white matter changes.
This study shows that the more lesions in the outer part of your brain in the grey matter, the more likely you are to accumulate disability, so the more active your disease is the more disability is accumulated. This study indicates that grey matter lesions are more sensitive to detect disability than white matter lesions. whilst it suggests that this may occur independently, loss of axons in the white matter, with lead to loss of neuron cell bodies in the grey matter. However damage in the white matter is masked because of the presence of more marked inflammation and the presence of swelling that may interfere with interpretation of imaging.
Thus, a 5-year prospective longitudinal study was carried on in a large group of patients with multiple sclerosis. Three hundred and twelve consecutive patients with multiple sclerosis (157 relapsing remitting, 35 paediatric, 45 benign, 44 primary progressive and 31 secondary progressive) were enrolled in a 5-year prospective clinical and neuroimaging study. Several magnetic resonance parameters (including cortical lesion number and volume, contrast-enhancing cortical lesions and grey matter atrophy) were analysed to find associations with clinical and cognitive outcomes.
Patients with high cortical lesion load (a lot of Grey matter lesions) had higher Expanded Disability Status Scale increase (median = 1.5; range = 0-3. More movement disability) during the study than both patients with low cortical lesion load (median = 1.0; range = 1-3, P < 0.001) and without cortical lesions (median = 0.5; range = -1 to 2, P < 0.001). Compared with clinically stable patients, 101 (32.4%) patients showing clinical progression at 5 years had the highest rate of cortical lesion accumulation (P < 0.001. The more active is your MS the more disability that is accumulated). Stepwise regression analysis revealed significant and independent contributions from age (β = 0.55), cortical lesion volume (β = 0.58), T2 white matter lesion volume (β = 0.34) and grey matter fraction (β = 0.42) as predictors (final model with r2= 0.657, P < 0.001) of Expanded Disability Status Scale change (Age, Size of White and Grey Matter lesions are predictors of mobility). Disease duration (β = 0.52, P < 0.001), cortical lesion volume (β = 0.67, P < 0.001), grey matter fraction (β = 0.56, P < 0.001) and T2 white matter lesion volume (β = 0.31, P = 0.040) at baseline were found to be independent predictors of cognitive status at the end of the study (The longer you have had disease and grey and white matter lesion load are predictors of disability years later)
While confirming the relevance of cortical pathology in all multiple sclerosis phenotypes, but benign, our study suggests that grey matter and white matter changes in multiple sclerosis occur, at least, partly independently, and that grey matter, more than white matter, damage is associated with physical and cognitive disability progression. Thus, the combination of grey and white matter parameters gives a more comprehensive view of multiple sclerosis pathology and allows a better understanding of the progressive phase of the disease, which, however, seems more related to cortical damage than to subcortical white matter changes.
This study shows that the more lesions in the outer part of your brain in the grey matter, the more likely you are to accumulate disability, so the more active your disease is the more disability is accumulated. This study indicates that grey matter lesions are more sensitive to detect disability than white matter lesions. whilst it suggests that this may occur independently, loss of axons in the white matter, with lead to loss of neuron cell bodies in the grey matter. However damage in the white matter is masked because of the presence of more marked inflammation and the presence of swelling that may interfere with interpretation of imaging.